Introduction
This tutorial will take you through a basic introduction to the renin-angiotensin-aldosterone system, or RAAS.
You will navigate through this tutorial using the buttons at the top of the screen.
The tutorial will ask you questions. Click on your chosen answer to see feedback; click the answer again to make the feedback disappear. When you're finished with one page, click the navigation button for the next page to move ahead.
Have fun! Click on button '1' to see the first page of the tutorial.
Page 1
The Renin-Angiotensin-Aldosterone System is one of the most important pathways in your body. It's part of the vital Generalized Stress Response that you use to survive injuries and emergencies.
But what turns it on? Choose the best answer. To hide the feedback, just click on the answer again.
Page 2
Good work! The Renin-Angiotensin-Aldosterone System will turn on when your blood pressure drops.It's often activated by the Sympathetic System, your 'fight or flight' response. But it can be activated by another organ too. The first word gives you a clue.
Page 3
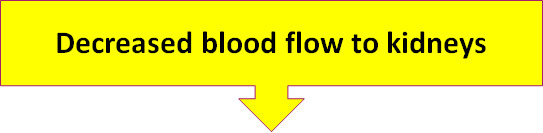
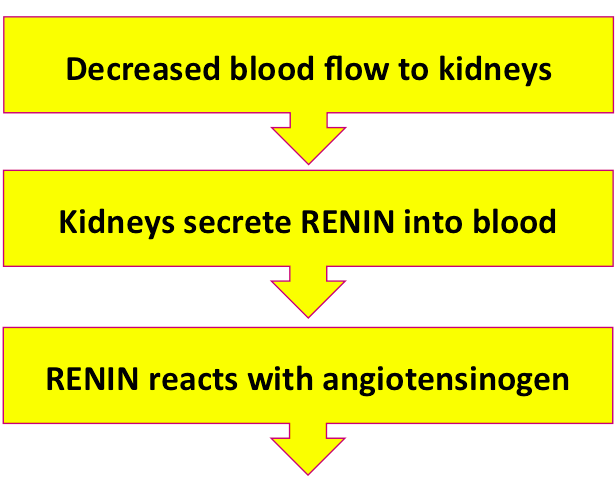
That's right! decreased renal blood flow will alert the kidneys to your decrease in blood pressure. This means that sometimes the kidneys make a mistake. If your renal arteries were blocked, for instance, the kidneys would always be turning on the RAA System, even if your blood pressure was fine.
What will the kidneys do when they sense decreased renal blood flow?
Page 4
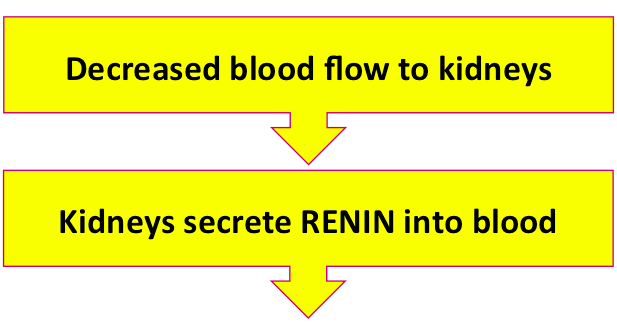 Good work! Renin is secreted into the blood, but it doesn't directly influence other cells. Instead, it interacts with another protein in the blood.
Good work! Renin is secreted into the blood, but it doesn't directly influence other cells. Instead, it interacts with another protein in the blood.
What could that protein be? The system's name gives you a clue.
Page 6

Good work so far!
This first angiotensin is called Angiotensin I. You will see a different kind of angiotensin later.
What would something called 'Angiotensin' do to help raise blood pressure?
Page 7

Angiotensin I constricts blood vessels in the other tissues, so the systemic vascular resistance (peripheral resistance) will increase -- and so will the blood pressure, and the flow of blood to the kidneys. But it isn't a very strong vasoconstrictor, so the body turns it into another compound that is stronger. What might that compound be?
Page 8
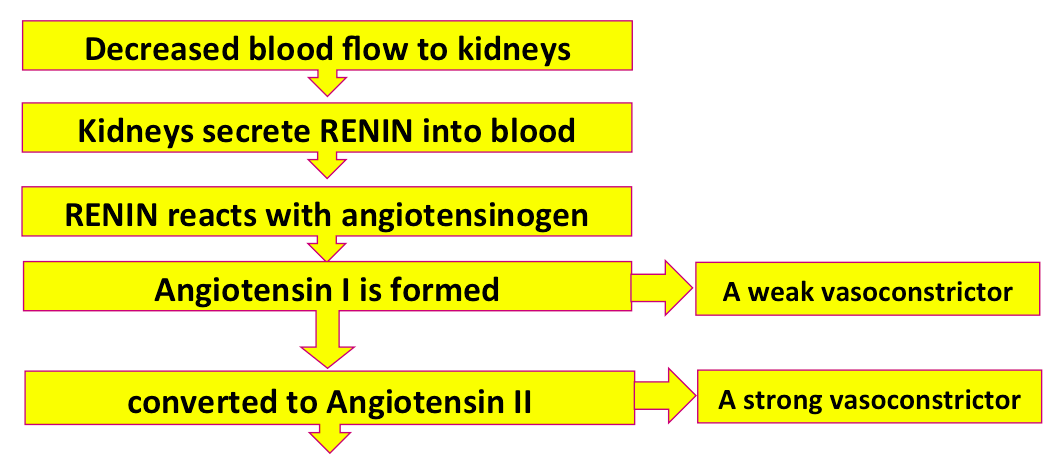
Angiotensin II is a much stronger vasoconstrictor. It can raise the blood pressure higher, increase renal blood flow, and make the kidneys happier. What would you call the enzyme that converted the angiotensin I into angiotensin II?
Page 9
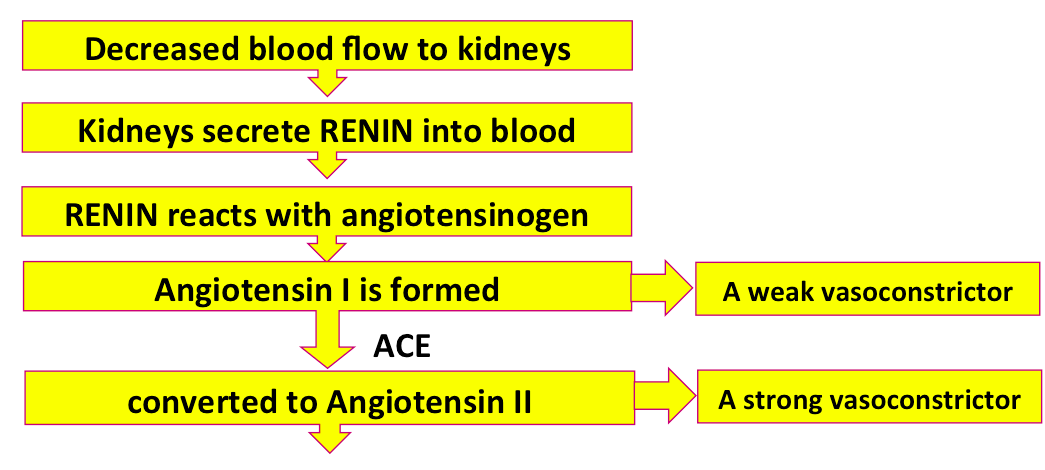
Angiotensin Converting Enzyme is so important in this pathway that some people with high blood pressure are given drugs to block it - ACE inhibitors.
Now let's think about anatomy a little bit. The renin is released into blood in the renal venules, and it mixes with the blood and reacts with angiotensinogen to make angiotensin I. Where in the body should the Angiotensin Converting Enzyme be located, to make sure it reacts with the most angiotensin I?
Page 10

Since all the blood in your body has to return to the right heart and be sent through the lungs, ACE located in the lungs will be able to affect lots of the Angiotensin I.
Now that Angiotensin II has been produced and is constricting vessels and raising the blood pressure, the kidneys' problem might be solved. But what's happening to the other organs?
Page 11

The kidneys might be happy, but the other organs will not be! What's a good long-term solution?
Page 12

To recap: There wasn't enough blood reaching the kidneys, so they increased their RENIN secretion to turn up the RAAS. That caused more of angiotensin I and II to form, and those compounds constricted blood vessels, raising BP. But there still wasn't enough blood, so now the body needs to increase blood volume. Angiotensin II starts this process by stimulating a gland just above the kidneys.
What gland would that be?
Page 13

Good work! Angiotensin II alerts the adrenal cortex to increase blood volume.
But the adrenal cortex is just a gland - it doesn't have any ability to directly increase blood volume. Instead, it uses the hormone aldosterone to turn on something that DOES have the ability to increase blood volume.
What is the aldosterone likely to activate?
Page 14
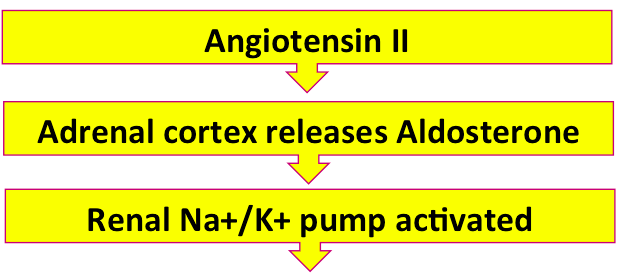
The Na+/K+ ATPase in the kidneys controls the movement of ions between the urine and the blood.
Do you remember which way it moves which ion?
Page 15
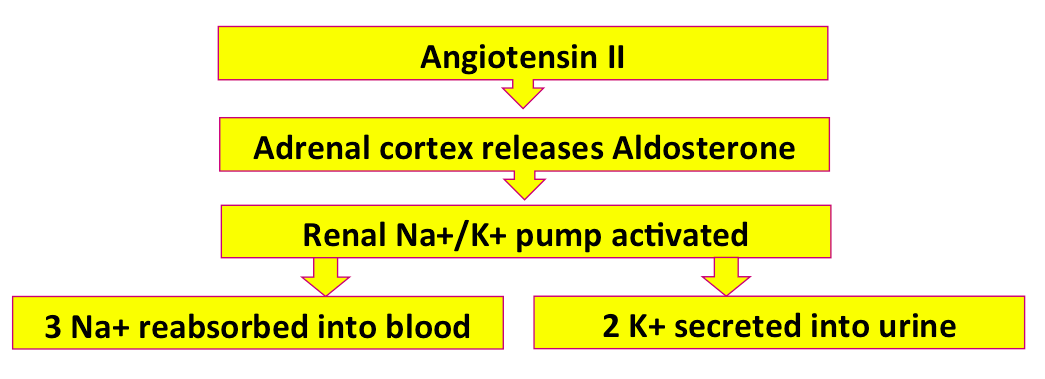
The renal Na+/K+ ATPase is just like the Na+/K+ ATPase in your cells. It moves 3 Na+ from urine to blood and 2 molecules of K+ from blood to urine. In kidney physiology, we say the Na+ is 'reabsorbed' and the K+ is 'secreted'.
Which way will water move?
Page 16
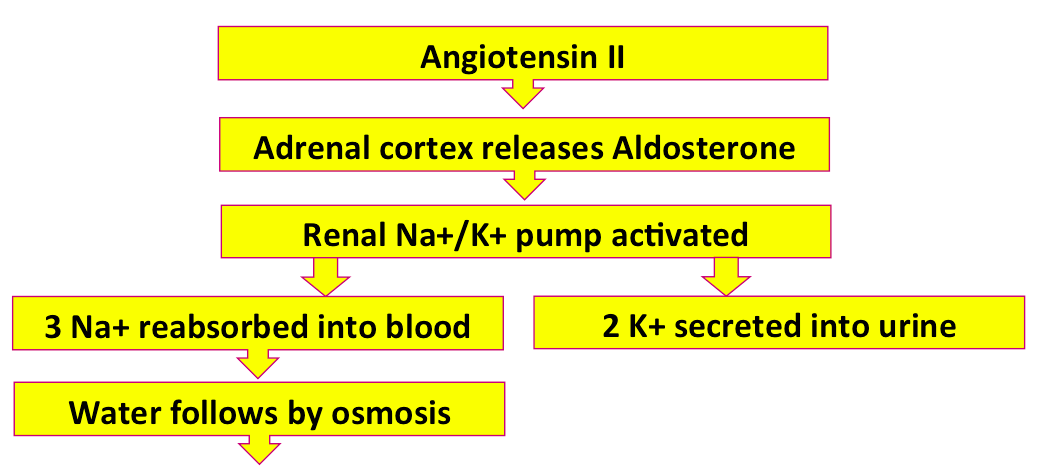
When the 3 Na+ are reabsorbed into the blood, water will follow by osmosis. This will increase blood volume.
How will this movement of water and solutes into the blood change blood tonicity (osmolarity)?
Page 20
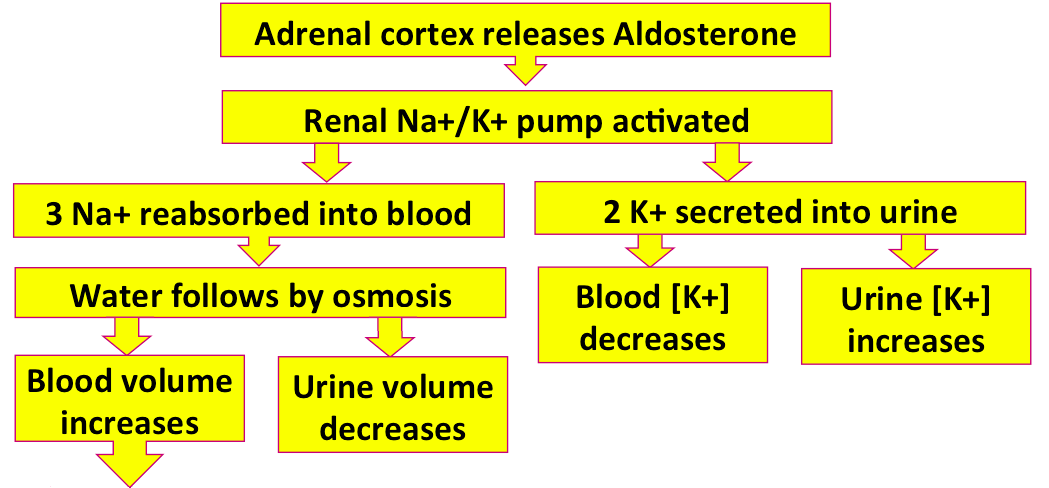
How will all this affect the kidneys?
That was a long pathway! This would be a good time to review it with a little quiz.
Page 21
Click on the correct answer from each set of options. Good luck!The kidneys start the RAAS pathway when their Blood flow drops / O2 supply drops . They increase their secretion of rennin / renin .
As a result, the protein Angiotensinogen / Angiotensin I is converted into Angiotensin I / Angiotensin II . This protein is a vasodilator / vasoconstrictor . When it passes through the kidneys / lungs , it is converted to the stronger compound Aldosterone / Angiotensin II by the enzyme ACE / ADH .
While Angiotensin II / Renin is a stronger vasoconstrictor, its even more important function is to stimulate the kidneys / adrenal cortex to release more Cortisol / Aldosterone . This hormone activates the Na+ channels / Na+/K+ ATPase in the heart / kidneys , causing it to move 3Na+ / 2K+ from the urine into the blood and 3Na+ / 2K+ from the blood into the urine. Water moves from the blood into urine / urine into blood because of osmosis / electric attraction .
While this system is running, blood volume will increase / decrease and urine volume will increase / decrease . In addition, blood [K+] will increase / decrease .
Blood osmolarity will increase / decrease / stay the same , because solutes moved into the blood / water moved into the blood / both solutes and water moved into the blood .
Now that the blood volume has increased / decreased , the kidneys will make more renin / make less renin , because they are getting enough blood / getting enough O2 .
Does the secretion of renin and aldosterone stop completely? Yes, the pathway's over / No, there's always some secretion.
Page 22
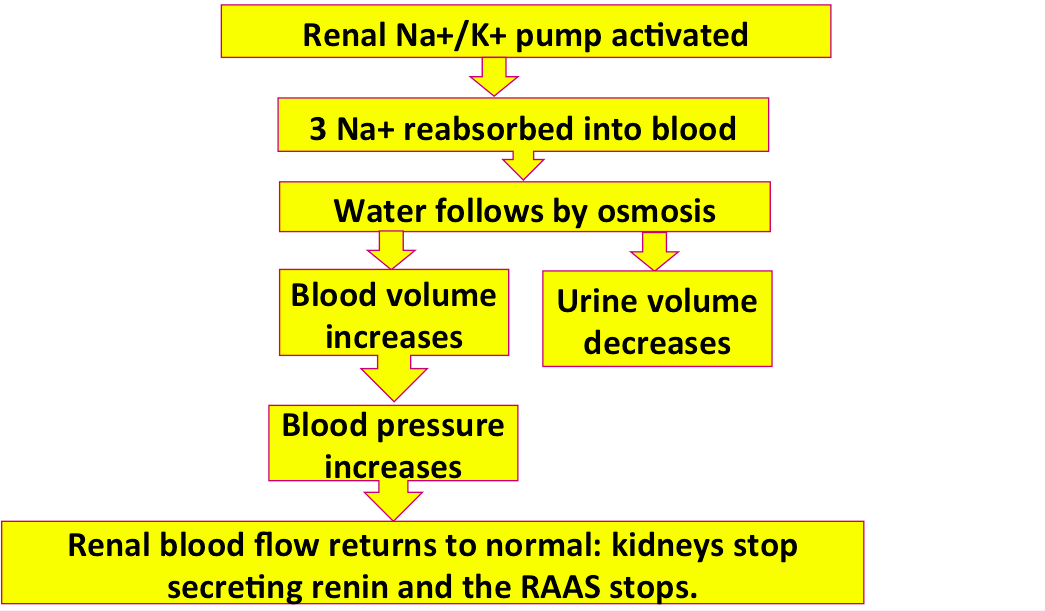
This is the end of the pathway. It started when the kidneys didn't have enough blood, and now it's fixed that problem and the kidneys have stopped secreting extra renin.
There's one other thing you should know. While the kidneys can make the adrenal cortex secrete aldosterone through the RAAS, there are other times the adrenal cortex secretes aldosterone all on its own. When do you think the adrenal cortex ought to secrete aldosterone?
You're done now, and should be able to apply this information to the cases on the next page!
Page 23
For each of these people, predict what will be happening to their RENIN, ANGIOTENSIN, and ALDOSTERONE levels, blood pressure or volume, and blood K+. To see the correct answers, just click on the patients. Mr. A has low blood pressure and high blood K+Mrs. B has high blood pressure and high blood K+
Mr. C has way too much aldosterone
Ms. D has high blood pressure and is taking an ACE inhibitor
Mr. E cannot run the renal Na+/K+ ATPase
Ms. F has high blood pressure and a clot blocking one of her renal arteries
Congratulations on completing the RENIN-ANGIOTENSIN-ALDOSTERONE SYSTEM tutorial! This is just one of the responses your body uses to handle stress. The others are the Sympathetic Nervous System, the Corticotropin Releasing Hormone System, and Antidiuretic Hormone. You can reach them by clicking on their names.
Material for this activity is taken from:
Fox, S.I. (2013) Human Physiology, 13th ed., McGraw-Hill
 And what will it make?
And what will it make?

